Spinal Cord Stimulation (SCS), a form of neuromodulation, can be used to treat certain chronic, intractable pain conditions that have not responded to more conservative approaches such as medication, surgery, manual therapy, exercise or psychological interventions.
Despite being considered minimally invasive, it is not without risk and is considerably expensive.
Having been in use for over 50 years, the technology is evolving at a fast pace, with newer approaches targeting different anatomical structures and using differing forms of stimulation.
However, the overall success rate associated with the use of the technique has not improved over recent times. (1)
What Does It Involve?
There are several different types of SCS, but generally it involves the placement of specialised electrodes into the epidural space or around the dorsal root ganglion.
It is typical to trial SCS before implantation. This is done via percutaneous leads, connected to an external battery. This allows the patient to experience stimulation, and gauge their response to the therapy.
If the patient responds, then a complete system is implanted, which consists of:
- Leads/electrodes (either surgical leads, which require a laminotomy to insert, or percutaneous leads, which can be inserted through a needle)
- Anchors (fastening sleeves to hold the leads in place)
- Implantable Pulse Generator (IPG)
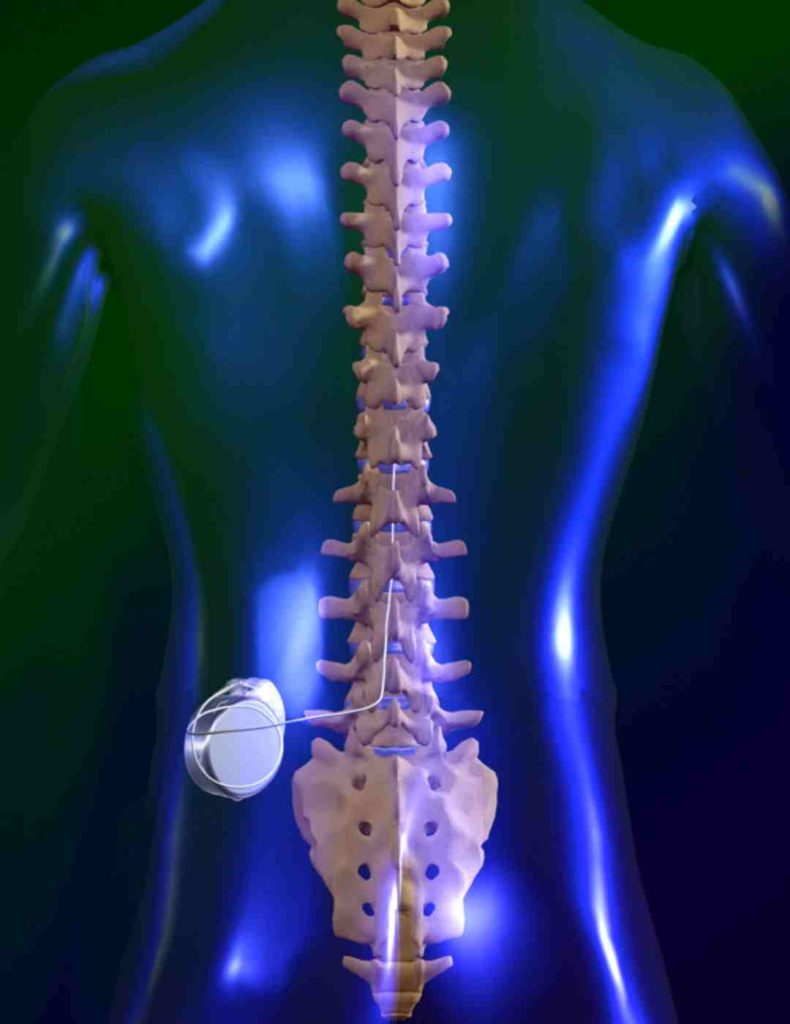
The electrodes connect to the implantable pulse generator (IPG), which is similar to a cardiac pacemaker in size and shape. This is typically implanted in the lower back or flank, though sometimes it is place in the abdomen.
The system is then programmed to deliver electrical current to the spinal cord or nerves, like a TENS machine. The system is programmed via a wireless connector through the skin, with the information stored on internal memory inside the IPG.
There are both rechargeable and non-rechargeable (primary cell) IPGs on the market, with advantages and drawbacks to both. Charging is done via a wireless charger, similar to a mobile phone charger.
How Does It Work?
The electrodes generate electrical fields between them and the change in charge influences the nervous tissue in the vicinity, causing either depolarisation or hyperpolarisation of neruons.
It is thought to provide pain relief via several mechanisms.
Early stimulation with some reference to Melzack and Wall’s gate control theory via tonic stimulation of the dorsal column. This involved the patient experiencing parasthesia over the pain area, masking their pain.
Newer paradigms involve multiple waveforms and frequences, with different anatomical targets, such as the dorsal horn. These forms of stimulation can be delivered at sub-parathesia thresholds, and still provide pain relief.
Areas of the nervous system known to be affected in successful SCS stimulation include the dorsal columns of the spinal cord, supraspinal regions and higher order processing within regions of the cortex. Other, more recently reported effects of SCS have been identified in glial cells and descending modulatory systems. Despite a great deal of research on the topic, it is fair to say that the exact mechanisms regarding the efficacy of SCS are still fairly hazy. (2)
What are the indications?
Its main use of SCS is for intractable pain conditions.
Because of the invasive and expensive nature of SCS, it is not used unless the indications for it are clear, and even then, typically after all other approaches have been exhausted.
The patients who are candidates for SCS are often in debilitating pain and experience a great deal of associated suffering and disability. This is not an approach for your garden variety back pain!
Neuropathic pain is the most common indication and some of the conditions include:
- Failed back surgery syndrome – chronic back pain following any type of invasive lumbar surgery such as laminectomy or fusion surgery.
- Chronic Regional Pain Syndrome (CRPS) of a single limb
- Chronic migraines
- Chronic pelvic pain
Other Applications of SCS
There is a growing area of research for the use of SCS with people who have sustained a spinal cord injury in order to restore some motor function. We won’t discuss this beyond mentioning it.
Does it work?
To answer this question, first we need to define work.
When we are talking about the efficacy of treating chronic pain, the parameters generally used to define success are a reduction of pain on a VAS scale by 30-50%.
Understanding expectations are really important in this field as miracle cures and complete pain relief are fairly infrequent. Whilst most people might consider a 30% reduction in pain to be insufficient, on a more functional level it may mean the difference between a person being able to tolerate being in the car for an hour compared to just 10 minutes, or a reduction or cessation of opioid or other medications which carry with them a whole lot of life interfering side effects of their own.
Tread Carefully With The Evidence
There are few true placebo SCS studies. This means it is hard to know the magnitude of the specific effect of spinal cord stimulation on pain and function.
Because parasthesia based stimulation was the dominant method for the majority of SCS history, it was traditionally hard to conduct a double-blinded trial. Hence, we must interpret the studies with caution.
It’s also important to note that the multifactorial nature of pain means that some people are likely to respond to SCS better than others. This is likely due to the pain being mediated by other factors not related to the nervous system itself. Factors that are known to reduce the chances of SCS being effective include depression, PTSD, the presence of third party compensation, misuse of alcohol or other drugs, low self efficacy and other evidence of poor coping skills (3, 4).
Without boring you to death with an extensive review of the literature, it would be fair to say that around half of the people implanted with SCS, regardless of the system used, the type of lead placement or the differing use of electrostimulation types (burst, frequencies etc.) achieve a reduction in their pain of between 30 and 50%.
This reduction in VAS scores goes hand in hand with increases in function and quality of life. In practice, having a skilled operator is likely to increase the chances of success and reduce complication rates, and some influential clinicians are aiming for 80/80 – an 80% pain reduction in 80% of patients, given the improving technology and optimal patient selection, which is going to give the best success rates for a particular clinic (1, 4, 5).
More Than Numbers
In the pain clinic setting, the suffering that often goes hand in hand with neuropathic pain can be almost unquantifiable.
Ordinary people who are unlucky enough to be afflicted with this condition in its variable forms tend to say very similar things about their situation and often follow an understandable downward spiral of loss of function and increasing misery.
The depression and fear avoidance with movement that frequently accompanies the suffering are the target of the allied health team working with these patients. Whilst they are frequently modifiable to a degree, they are also incredibly understandable given the situation.
The desire to have an option to at least try to ease suffering is the obvious rational for the use of SCS in the pain clinic setting, despite its lack of overwhelming efficacy. When it goes well, it changes lives.
References
1. Sdrulla AD, Guan Y, Raja SN. Spinal Cord Stimulation: Clinical Efficacy and Potential Mechanisms. Pain Pract 2018;18:1048-67.
2. Vallejo R, Bradley K, Kapural L. Spinal Cord Stimulation in Chronic Pain: Mode of Action. Spine (Phila Pa 1976) 2017;42 Suppl 14:S53-60.
3. Blackburn DR, Romers CC, Copeland LA, Lynch W, Nguyen DD, Zeber JE, Hoffman MR. Presurgical Psychological Assessments as Correlates of Effectiveness of Spinal Cord Stimulation for Chronic Pain Reduction. Neuromodulation 2016;19:422-8.
4. Prabhala T, Kumar V, Gruenthal E, Collison C, Prusik J, Owusu S, et al. Use of a Psychological Evaluation Tool as a Predictor of Spinal Cord Stimulation Outcomes. Neuromodulation 2019;22:194-9.
5. Brinzeu A, Cuny E, Fontaine D, Mertens P, Luyet PP, Van den Abeele C, et al. Spinal cord stimulation for chronic refractory pain: Long-term effectiveness and safety data from a multicentre registry. Eur J Pain 2019;23:1031-44.
